Current Research
A SYMPTOM TO CIRCUIT APPROACH TO UNDERSTAND AUTISM
- How are cortical circuits assembled during typical brain development?
- What are the underlying circuit defects in autism and intellectual disability?
- What are the best ways to model neuropsychiatric symptoms?
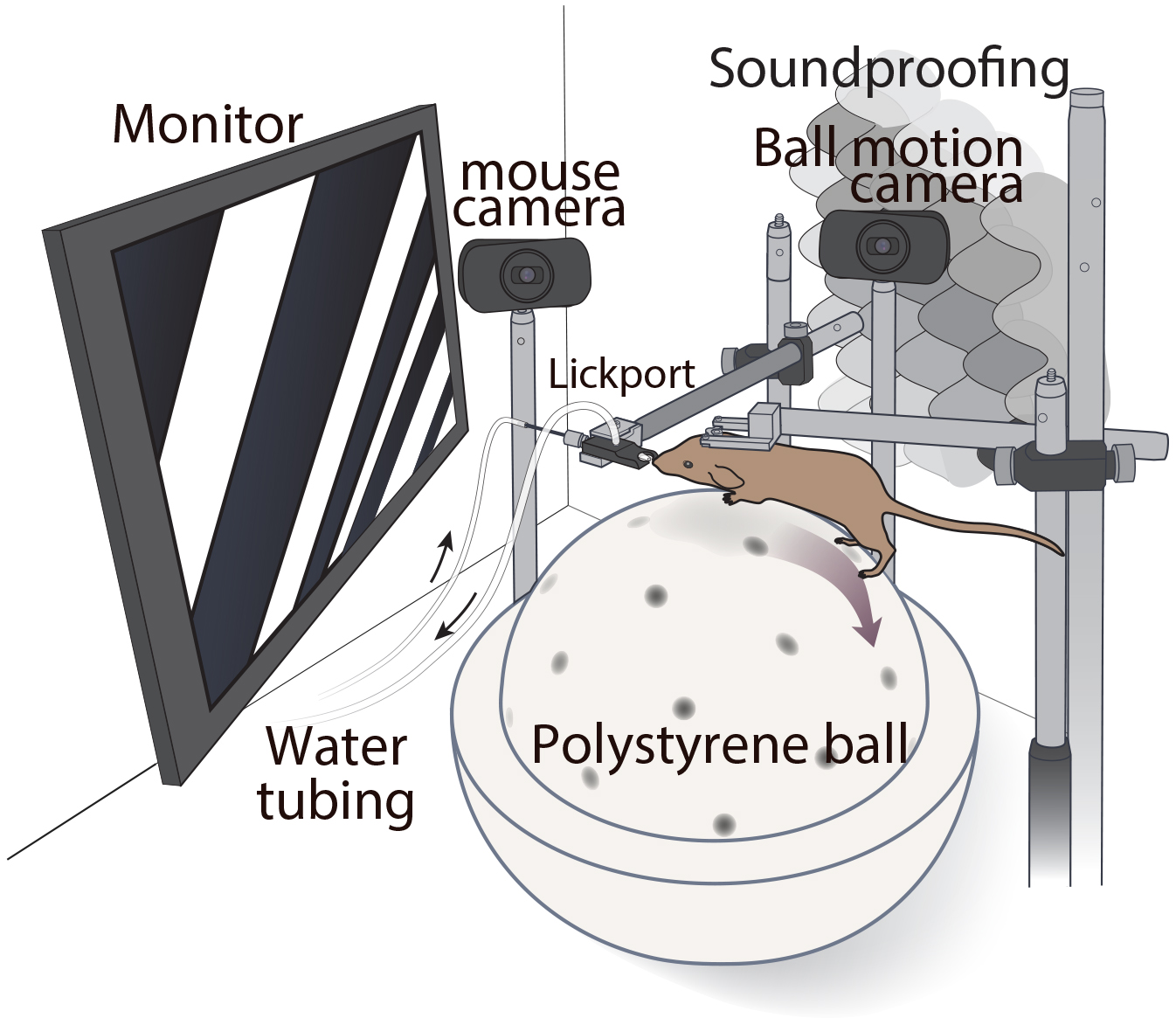
We are trying to answer these questions using the latest state of the art tools in neuroscience research, such as in vivo 2-photon calcium imaging and silicon probes to record network activity, chemogenetics with DREADDs or optogenetics to manipulate neuronal activity, and sophisticated behavioral tasks.
Our research is particularly relevant to neuropsychiatric disorders that lack distinct neuropathological features and are therefore more likely caused by subtle alterations in how neuronal activity propagates across brain circuits.
The traditional approach to understand how symptoms arise in complex neuro-psychiatric disorders has been to start at the molecular level and use gain- or loss-of-function manipulations of a given pathway to correct synaptic defects and/or abnormal mouse behavior. Unfortunately, this approach has often overlooked potential circuit alterations that could link the molecular/synaptic defects with the behavioral phenotype, which may explain why so far it has had limited translational potential.
Instead, we have adopted a symptom-to-circuit approach to reverse engineer how different symptoms in neurodevelopmental disorders arise from specific network level disruptions in neuronal connectivity and function.
Rather than relying on traditional behavioral assays (such as marble burying, elevated plus maze or three-chamber assay) that have not been–or cannot ever be–validated in humans, we are implementing analogous perceptual learning tasks in both humans and experimental models of autism.